Making the Syphi-list
New STD data keeps D.C. in the top 25
Recently released data from the Centers for Disease Control and Prevention (CDC) tracking sexually transmitted diseases in 2003 does not offer much good news for men who have sex with men (MSM). The primary low point is with syphilis, on the rise within the MSM community, but declining within other populations.
“After an all-time low in 2000, the syphilis rate in the U.S. rose for the third consecutive year in 2003, increasing 19 percent during the three-year period,” the CDC states in its data summary. “Outbreaks of syphilis among MSM have been reported in several U.S. cities in recent years, and are believed to be largely responsible for the increasing national syphilis rate. Recent CDC research suggests that more than 60 percent of all [primary and secondary syphilis] cases reported in 2003 occurred among MSM.”
The news isn’t much cheerier where gonorrhea is concerned. The CDC reports that the disease is at an “all-time low,” but cautions that it is likely underreported. In 2003, there were 335,104 reported cases of gonorrhea. However, the CDC estimates 718,000 cases annually.
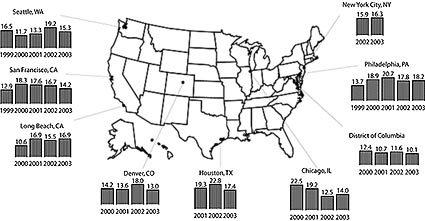 |
Of particular interest to gay men is news of hard-to-treat strains of gonorrhea. “Antimicrobial resistance is an increasingly important concern in the treatment and prevention of gonorrhea, particularly for the MSM,” according to the CDC, adding that overall, fluoroquinolone-resistant gonorrhea appear in 4.1 percent of cases in 2003, up from 2.2 percent in 2002 and 0.7 percent in 2001. Fluoroquinolones are a type of antibiotic — one common form is ciprofloxin, marketed as Cipro.
Among MSM, the appearance of antibiotic-resistant gonorrhea jumps to 15 percent of reported cases.
“In April 2004, CDC recommended that fluoroquinolones no longer be used as treatment for gonorrhea in MSM,” the report summary notes. “In addition, in California and Hawaii, where resistant cases have been widespread for several years, and in Washington [State], where resistant cases have appeared more recently, fluoroquinolones are no longer recommended to treat any cases of gonorrhea. The currently available antibiotics recommended by CDC for treatment of fluoroquinolone-resistant gonorrhea are expensive and must be administered by injection, instead of taken orally.”
Regarding chlamydia, the news remains largely the same — it “remains the most commonly reported infectious disease in the United States.” The CDC recorded 877,478 infections in 2003, and increase of about 43,000 over 2002. The CDC says that in reality, the annual infection rate is nearly 3 million cases. This disease is most common in young women, and is the primary STD concern among lesbians. Still, men are often asymptomatic carriers. And as with any STD, chlamydia can make it easier for a carrier to become infected with HIV.
Some of the newly-released data has been broken down by city. For example, D.C. came in 14th in a ranking of cities with the highest rates of syphilis. That translates to 48 reported cases in 2003, or 8.4 cases per 100,000 residents. San Francisco was at the top of the list with 332 reported cases, or 43.5 per 100,000 residents.
In Washington, much of the CDC data regarding MSM was culled from Whitman-Walker Clinic. Patricia D. Hawkins, associate executive director of the clinic, has reviewed the summary of the CDC survey, and says she is not surprised.
“We’ve known that he syphilis rates were going up within the MSM community,” Hawkins says. “We’ve been trying to raise awareness, especially with people coming in for repeat STDs.”
Hawkins does not spend much time talking about syphilis or other STDs for their own sake, but zeroes in on STDs’ link to HIV. She says she worries that the rise in STDs is an alarming indicator that safe sex is waning in the MSM community. She cites two reasons for the perceived lapse.
The first is the medical advances that have allowed people to view HIV as a chronic, manageable infection, coaxing them to let their guard down, she says. The second reason is that a new generation of MSM have not witnessed AIDS-related death on the same scale as their forebears.
“Up till 1995, you couldn’t walk down 17th Street without seeing people who were wasting, using canes,” Hawkins recalls. “And people had lost people. I know young people who have never lost anyone to HIV, so the message isn’t as personal. And the people who die now, they usually die relatively quickly.”
After 20 years of safer sex, Hawkins, a psychologist, is no stranger to safe-sex burnout. She hopes that new programs in the works designed to help MSM negotiate sexual boundaries within a realistic context may be applied in D.C. Hawkins says that she’d be happy to simply see more condom use during anal sex among men, even if oral sex contains HIV/STD risk.
“If I were a gay man, I would certainly be much more worried about contracting HIV than syphilis, so syphilis is just a marker for us,” Hawkins reasons. “And my sense is that a lot of the syphilis we’re seeing is not coming from oral sex.”
Support Metro Weekly’s Journalism
These are challenging times for news organizations. And yet it’s crucial we stay active and provide vital resources and information to both our local readers and the world. So won’t you please take a moment and consider supporting Metro Weekly with a membership? For as little as $5 a month, you can help ensure Metro Weekly magazine and MetroWeekly.com remain free, viable resources as we provide the best, most diverse, culturally-resonant LGBTQ coverage in both the D.C. region and around the world. Memberships come with exclusive perks and discounts, your own personal digital delivery of each week’s magazine (and an archive), access to our Member's Lounge when it launches this fall, and exclusive members-only items like Metro Weekly Membership Mugs and Tote Bags! Check out all our membership levels here and please join us today!